 The Safety of Bioidentical Hormones by Jeffrey Dach MD
The Safety of Bioidentical Hormones by Jeffrey Dach MD
Bio-identical hormones exist naturally in the human body, so it is axiomatic that these are safe. However, we are interested in a slightly different question. What is the safety of bio-identical hormones as routinely used in medical practice? Let’s try to answer this question.
Left Image: Water with Droplets Courtesy of Wikimedia Commons. Author: Roger McLassus, CC 3.0.
A 50 Million Year Medical Experiment
The answer to the safety question is that bio-identical hormones are found in the human body naturally. Any harmful substance in the human body would impair survival, and over millions of years of evolution would be eliminated by natural selection. This is the basic concept of Darwinian evolution which is accepted by mainstream medical science. Consider the following medical experiment, bio-identical hormones, estrogen, progesterone, testosterone have been present in mammals for at least 120 million years, and primates for 60 millions years. Us primates are still here on the planet. I would consider that a successful medical experiment, wouldn’t you? For more, see What’s Wrong with Darwinian Evolution. (2)
Either Excess or Deficiency of Anything Can be Harmful
One of our routine labs tests called the Chem Panel measures electrolytes and glucose levels in the blood. The body automatically maintains these within narrow ranges to maintain health. If levels deviate above or below these normal ranges, this causes a serious health disturbance. For example elevated potassium levels causes cardiac arrest. Magnesium deficiency causes muscle spasm and arrhythmia. Excessive amounts of Vitamins A and D can lead to toxicity. Hormones levels enjoy a considerably wide range of acceptable limits.
Safety of Progesterone
When it comes to progesterone, levels during third trimester of pregnancy may reach 150 ng/ml, about 15 times higher than luteal phase progesterone levels in young females which plateaus at 10–20 ng/ml. Remember the fetus is bathing in this high progesterone dosage, as well. What this means is that extremely high serum levels of progesterone are perfectly safe. Administration of even very large doses of progesterone do not come close to reaching the levels of pregnancy. Having said this, oral progesterone taken during the daytime may induce sedative effect which may be annoying if the patient needs to stay alert during the day. In addition there may be very rarely an allergic response to high doses of progesterone. Also, administration of insufficient doses of progesterone may induce a paradoxical worsening of PMS symptoms or peri-menopausal symptoms, usually relieved by increasing the progesterone dosage. For more on this, see: Progesterone Safety and Adverse Effects. (80-86)
However, a deficiency or excess of estrogen, or a deficiency of progesterone may produce symptoms. This is called estrogen deficiency/excess, and progesterone deficiency, and they each have typical signs and symptoms easily recognized.(3)
Common Signs of Estrogen Deficiency (4)
Mental fogginess
Forgetfulness
Depression
Minor anxiety
Mood change
Difficulty falling asleep
Hot flashes
Night sweats
Temperature swings
Day-long fatigue
Reduced stamina
Decreased sense of sexuality
Lessened self-image and attention to appearance
Dry eyes, skin, and vagina
Loss of skin radiance
Feel balanced 2nd part of cycle
Sagging breasts and loss of fullness
Pain with sexual activity
Weight gain
Increased back and joint pain
Episodes of rapid heartbeat
Headaches and migraines
Gastrointestinal discomfort
Constipation
Common Signs of Excess Estrogen (takes longer to notice)
Breast tenderness or pain
Increased breast size
Water retention, fingers, legs
Impatient, snappy behavior, but with clear mind
Pelvic cramps
Nausea
Common Signs of Progesterone Deficiency
No period at all (no ovulation)
The period comes infrequently (every few months)
Heavy and frequent periods (large clots, due to buildup in the uterus)
Spotting a few days before the period. (Progesterone level is dropping)
PMS
Cystic breasts
Painful breasts
Breasts with lumps
Most cases of endometriosis, adenomyosis, and fibroids.
Anxiety, irritability, nervousness and water retention
Above list can be found in the book, Natural Hormone Balance for Women by Uzzi Reiss MD (4)
Testosterone for Women: Signs and Symptoms of Testosterone Deficiency/Excess
Testosterone for women is a major breast cancer preventive, based on the work of Rebecca Glaser MD, a breast surgeon in Dayton Ohio who treats menopausal women with testosterone pellets. For more on this see: Testosterone For Prevention and Treatment of Breast Cancer.
Signs and Symptoms of Testosterone Deficiency:
Loss of libido
Low motivation
Fatigue
Loss of muscle mass (sacopenia)
Loss of bone density (osteopenia, osteoporosis)
Cognitive Dysfunction
Mood disturbance
Dry Skin
Dry Eye Syndrome
Increased Risk for Breast Cancer
Signs and Symptoms of Testosterone Excess
Excess oily skin
Acne (pimples)
Excess or aggravation of facial hair
Excess libido
Aggression, hostility, mood disturbance
Relieving Symptoms of Hormone Excess
For those patients using topical or vaginal hormone delivery experience excess symptoms, simply take a break from using the hormone preparation for 3-7 days. Once symptoms resolve, resume the hormone treatment at half dosage.
Adverse Effects of NSAID Pills
Over-the-counter pain pills (NSAIDs) such as aspirin, naproxen and ibuprofen are considered fairly safe. After all, you don’t need a prescription to buy them. In 1999, Dr. Michael Wolfe studied the adverse effects of NSAID pills finding NSAID use is responsible for an estimated 16,500 deaths in the US annually, mostly from gastric bleeding. Compare this to no reported adverse events from bio-identical hormones in 2008, according to an FDA Press Conference on Bioidentical Hormones January, 2008. However, the discussion of adverse effects of exogenous hormone administration is more complicated that the above FDA conference recording, subject of much debate over decades in the medical community. For example, what are the benefits and adverse effects of hormones on the cardiovascular system, on the brain, on risk for breast cancer, on risk for all other cancer, on risk for blood clotting, etc? These and other questions are discussed in other chapters. (5-6)
 The Elephant in the Room
The Elephant in the Room
Of course, the elephant in the room is the question, does menopausal hormone treatment increase the risk for breast cancer? The answer to this question is more complicated than a simple yes or no, and requires us to evaluation individual hormone components, estrogen, progesterone and testosterone separately, as well as how they are used in combination. When thinking about the role of hormones in the mammalian body, one must look at the big picture. The way, hormones work together is analogous to a symphony with many gifted musicians playing different instruments to make beautiful music. A good menopausal hormone program uses combinations of hormones in the proper ratios to achieve the highest safety and efficacy. In addition, don’t forget the importance of diet, dietary supplements and avoidance of hormone disrupting chemicals.
 Do Bio-Identical Hormones Cause Breast Cancer? The French Cohort Study
Do Bio-Identical Hormones Cause Breast Cancer? The French Cohort Study
According to the 2008 French Cohort study by Dr. Agnes Fournier, there is no increased risk of breast cancer in women using the bio-identical hormone combination of estradiol and natural progesterone. However, breast cancer risk is increased with the estradiol/ synthetic progestin combination.
Synthetic Progestins Increase Proliferation, Act as Carcinogens
Synthetic progestins are carcinogenic via two mechanisms. Firstly, as suggested by Dr. Sebastián Giulianelli in 2012, progestins activate ER-alpha which together with the PR (progesterone receptor) activates Cyclin D1 and MYC oncogenes. Secondly as Dr. Steven Birrell suggests in 2007, synthetic progestins have androgenic properties which interfere with androgenic activation of ER-Beta, the tumor suppressor receptor. (40-44)
Testosterone Acts a Proliferative Brake
Dr. Birrell’s 2007 hypothesis was confirmed in 2014 by Dr. Aleksandra M. Ochnik who obtained normal breast tissue from surgical speciments and cultured the breast cells in presence of androgens (DHT) and MPA (medroxyprogesterone), finding Androgen, dihydrotestosterone, inhibits breast cell proliferation. MPA exerts an antiandrogen effect associated with increased proliferation and destabilization of the androgen receptor protein, writing:
DHT [Di-Hydro-Testosterone] inhibited the proliferation of breast epithelial cells in an AR-[Androgen Receptor] dependent manner within tissues from postmenopausal women, and MPA significantly antagonized this androgenic effect….In a subset of postmenopausal women, MPA exerts an antiandrogenic effect on breast epithelial cells that is associated with increased proliferation and destabilization of AR [Androgen Receptor] protein. This activity may contribute mechanistically to the increased risk of breast cancer in women taking MPA-containing EPT [estrogen-progestin therapy]. (87)
Upper Left Image: Eiffel Tower, Paris, France, Author Pinterpandai.com , Courtesy of wikimedia commons.
Progesterone Acts As Proliferative Brake
In 2015, Dr. Hisham Mohammed did a series of studies using in vitro and in vivo mouse xenografts, finding activation of the progesterone receptor (with exogenous progesterone) results in a “robust association between PR and the ERα complex” which then acts as a “proliferative brake” and blocks breast tumour growth in mouse xenografts. Dr. Hisham Mohammed also states the progesterone receptor “functions as a molecular rheostat to control ERα chromatin binding and transcriptional activity”. Remember, ER-alpha is the proliferative receptor, while ER-Beta is the protective one. In this scenario, progesterone receptor protein binds to ER-alpha and brakes (halts) ER-alpha induced proliferation, resulting in a good clinical outcome. Dr. Hisham Mohammed writes:
under estrogenic conditions, an activated PR [progesterone receptor] functions as a proliferative brake in ERα+ breast tumours by re-directing ERα chromatin binding and altering the expression of target genes that induce a switch from a proliferative to a more differentiated state … Our findings indicate that PR functions as a molecular rheostat to control ERα chromatin binding and transcriptional activity, which has important implications for prognosis and therapeutic interventions…the increased risk of breast cancer associated with progestogen-containing HRT is mainly attributed to specific synthetic progestins, in particular medroxyprogesterone acetate (MPA), which is known to also have androgenic properties. The relative risk is not significant when native progesterone is used. In ERα+ breast cancers, PR is often used as a positive prognostic marker of disease outcome4… progesterone treatment has been shown to be antiproliferative in ERα+ PR+ breast cancer cell lines and progestogens [natural progesterone, not progestins] have been shown to oppose estrogen-stimulated growth of an ERα+ PR+ patient-derived xenograft. In addition, exogenous expression of PR in ERα+ breast cancer cells blocks estrogen-mediated proliferation and ERα transcriptional activity…These observations imply that PR activation in the context of estrogen-driven, ERα+ breast cancer, can have an anti-tumourigenic effect. (73)
Note: ER-alpha is the proliferative, procarcinogenic receptor, while ER-beta is the tumor suppressor receptor.(40-54)
French Cohort Study
In 2008, Dr Agnes Fournier from Paris, France studied 80,377 postmenopausal women using various hormone replacement regimens for a mean duration of 8.1 years in the E3N/EPIC study using self administered questionnaires. Pathology reports for 2,354 cases of invasive breast cancer were reviewed in 96 percent of cases. Almost all (98 percent) of the women used estradiol, and only 2 percent used CEE (Premarin). Estradiol-alone users had a 29 percent increase in breast cancer due to proliferative effects of estradiol. However, the estradiol/progesterone combination group had no increase in risk for breast cancer compared to the general population, thus suggesting an anti-proliferative effect of natural progesterone. However, when a synthetic progestin is added to the estradiol, these women had a 69 percent increased risk for breast cancer. These results are similar to those of Dr. Charles Wood using a primate model of post menopausal hormone replacement. For more on primate hormone studies, see: Don’t Monkey with my Hormones. Dr. Agnès Fournier writes:
Recently, Wood et al. [22] compared the effects of estradiol given with either medroxyprogesterone acetate or micronized progesterone on risk biomarkers for breast cancer in a postmenopausal primate model. In this randomized crossover trial, they found that, compared to placebo, estradiol + medroxyprogesterone acetate resulted in significantly greater proliferation (as measured by Ki67 expression) in lobular and ductal breast epithelium, while estradiol + micronized progesterone did not. This result supports our findings suggesting that, when combined with an estrogen, progesterone may have a safer risk profile in the breast compared with some other progestagens. (8A-C) Note: the word “progestagens” used here refers to synthetic progestins.
In 2023, Drs. Gompel and Jerilynn Prior discuss the findings of the French Cohort Study (E3N-Cohort) in response to two publications by Drs. Bennink Coelingh and Dr. V. Craig Jordan proclaiming that erroneous statement that progesterone and not estrogens causes breast cancer. Of course, this is completely wrong. Drs. Gompel and Jerilynn Prior point to the French E3N Cohort study which shows 29 percent increased risk with estradiol alone. However, when natural progesterone is combined with the estradiol, this risk is abolished, writing.
the breast cancer results from an 8-year prospective observational study with more than 80,000 participants (in France called E3N cohort) which allowed a comparison of breast cancer risk on various single and combined menopausal hormonal therapies (MHT) [22]. This study documented breast cancer risk in untreated postmenopausal women as controls versus those taking MHT [Menopausal Hormone Therapy] with estradiol alone (risk ratio 1.29, 95% confidence interval 1.02, 1.65) versus estradiol plus progesterone (risk ratio 1.00, 95% confidence interval 0.83, 1.22). Although there was no increased breast cancer risk with estradiol–progesterone, estradiol with synthetic progestin MHT was related to significantly increased risk (risk ratio 1.69, 95% confidence interval 1.50, 1.91) [22]. A recent review [Hipolito, 2021] summarizes publications on a lower breast cancer risk in MHT of estradiol with micronized progesterone and dydrogesterone versus other progestins. (74-76)
E3N French Cohort Study, Agnes Fournier 2008
Estradiol Alone, or Estradiol with Progesterone:

Estradiol plus a progestin, either norethisterone or medroxyprogesterone:

The above two images courtesy of Table 2. Fournier, Agnès, Franco Berrino, and Françoise Clavel-Chapelon. “Unequal risks for breast cancer associated with different hormone replacement therapies: results from the E3N cohort study.” Breast cancer research and treatment 107 (2008): 103-111.
As mentioned above, the French Cohort is an observational study, not a randomized, placebo controlled trial (RCT). Whether or not estradiol alone increases or decreases risk of breast cancer is debatable in the medical literature over decades. Part of this debate relates to whether or not the menopausal patients studied have or have not been long term estrogen deprived as described by Dr. V. Craig Jordan as in the WHI study which transforms estrogen from a growth factor to a cancer death factor (apoptosis inducer). So, it would be nice to have other studies to confirm the French Cohort finding of increased risk of breast cancer for estradiol alone. HR=1.29 for estradiol alone, and HR=1.0 for combined estradiol/progesterone. Here are two supportive studies showing exactly that.
In 2006, Dr. Heli Lyytinen from Finland studied breast cancer risk in 84,729 post menopausal women using estrogen-alone therapy. Dr. Heli Lyytinen assumed the women started HRT at age 52, so they were not estrogen deprived. The breast cancer risk was increased 34 percent after 5 years of estradiol-alone use (HR=1.34), 57 percent for 10-20 years use, and 75 percent for greater than 20 years of use. Dr. Heli Lyytinen, writes:
we estimated the duration of estradiol use in women using estradiol since 1994 by assuming that they had started use at the age of 52 years, which is the case generally in Finland. The standardized incidence ratio related to estimated estradiol use of 5–10 years was 1.34 (95% CI 1.16–1.54; 193 observed cases of breast cancer), for use of 10–20 years 1.57 (1.31–1.86; 125 cases), and for use of more than 20 years, 1.75 (1.16 –2.55; 27 cases)…Estradiol for 5 years or more, either orally or transdermally, means 2–3 extra cases of breast cancer per 1,000 women who are followed for 10 years. (77-79)
In 2011, Dr. Kjersti Bakken studies the different types of menopausal hormone replacement and breast cancer risk in 133,744 women over 8.6 years of follow up who experienced 4312 primary breast cancers diagnosed, finding a 42 percent increased relative risk for current estrogen-alone use, writing:
The EPIC-cohort is a multicentre prospective cohort with 23 contributing centres in 10 European countries…We investigated the association between the use of different types of MHT and breast cancer risk…Approximately 133,744 postmenopausal women contributed to this analysis. Information on MHT was derived from country-specific self-administered questionnaires with a single baseline assessment. Incident breast cancers were identified through population cancer registries or by active follow-up (mean: 8.6 yr). A total of 4312 primary breast cancers were diagnosed during 1,153,747 person-years of follow-up…Compared with MHT never users, breast cancer risk was higher among current users of estrogen only (RR: 1.42, 95% CI 1.23–1.64). (77-79)
Of course, randomized controlled trials (RCT’s) are considered higher level of evidence than observational studies. In 2024 Dr. Rowan Chlebowski did a meta-analysis of 10 RCT’s of estrogen-alone and breast cancer incidence, finding a 23 percent reduction in breast cancer with estrogen alone. This 23 percent reduction is similar to the finding of the second arm of the WHI study using CEE (conjugated equine estrogen alone). Since I don’t have access to the entire article, I would suspect CEE was used, and I would ask if the patients were started later after a period of estrogen deprivation, all of which could influence the results. Dr. Rowan Chlebowski writes:
Findings from 10 randomized trials included 14,282 participants and 591 incident breast cancers….Combining the 10 trials, 3.6% (262 of 7339) vs 4.7% (329 of 6943) randomized to estrogen-alone vs placebo (overall RR 0.77 95% CI 0.65–0.91, P = 0.002). Conclusion: The totality of randomized clinical trial evidence supports a conclusion that estrogen-alone use significantly reduces breast cancer incidence. (79)
To be fair, one must mention the 2016 UK Generations Study by. Dr Michael Jones which also found no increased in breast cancer for estrogen-alone use (HR=1.0). However, this estrogen-alone study included mostly CEE use, which excludes this as an estradiol-alone study. (88)
Avoid Endocrine Disrupting Chemicals
We should mention here breast cancer prevention involves avoiding endocrine disrupting chemicals in the environment, Pthalates, Bisphenol-A and C, plastics etc. A good resource for learning about EDC’s (endocrine disrupting chemicals ) is Hormone Deception by Dr. Lindsey Berkson, and Our Stolen Future: Are we Threatening our Fertility, Intelligence, and Survival? by Theo Colburn. (9-10) (55-56)(89-94)
What Causes Breast Cancer ?
If estrogen/progesterone bioidentical hormone replacement does not cause cancer, then the next obvious question is what does cause breast cancer? Carcinogenic chemicals in the environment, water and food supply cause cancer. Here is a partial list of carcinogens in our food supply- Bisphenol A (BPA), Phthalates, Pesticides, Styrene, Vinyl Chloride, etc. When researchers wish to study breast cancer in mice, they induce breast cancer with the carcinogenic chemical DMBA, or the synthetic progestin medroxyprogesterone. (57-59)
Etiology of Breast Cancer in Humans
In humans, breast cancer is thought related to carcinogenic properties of estrogen metabolites called 4-hydroxy-quinones acting as DNA adducts causing oxidative damage to DNA. Normally estrogen is preferentially metabolized towards the favorable pathways leading to 2-MEO (2 methoxy-estradiol) which is cancer preventive. However, in some cases of nutritional deficiency, or genetic disorders involving methylation pathways, unfavorable 4-hydroxy quinones may accumulate in a bottleneck, thus increasing risk for breast cancer as suggested in 2021 by Dr. Ercole Cavalieri. That is where a knowledgeable doctor is helpful for laboratory tests and providing supplements such as iodine, DIM, methylfolate, selenium, resveratrol, N-acetylcysteine and vitamin D3 to reduce the risk for breast cancer. (60-62)
Do Bio-Identical Hormones Cause Heart Disease ?
Again, the answer is NO. A study of CAT calcium scores by JoAnn E. Manson in the June 2007 JAMA actually showed less heart disease in the women taking unopposed estrogen (they had hysterectomies and were not given the synthetic progestins).(11) These same results had already been published 2 years previously in a calcium score study by Budoff in J Womens Health 2005. (12)
A Closer Look at the Women’s Health Initiative WHI Study
Understanding the Women’s Health Inititative (WHI) study is not difficult, and is very important to answer the question of hormone safety. The WHI study was the large NIH sponsored medical study which compared synthetic hormones to placebo in two large groups of women. The WHI study consisted of two arms. The first arm used the synthetic hormones Premarin and Provera, and the second arm used Premarin alone.(13)(14)
What is Premarin and Provera?
Premarin and Provera are not bio-identical hormones. Premarin is a hormone obtained from pregnant horses, which contains Equilin, a horse hormone not found in humans.(15) Provera is a synthetic hormone which is not found anywhere in the natural world (see provera diagram below).(16) The Premarin and Provera combination is called PremPro, a synthetic hormone pill commonly prescribed by mainstream medicine. Prempro was the hormone preparation used in the first arm of the WHI study.(13)
WHI study First Arm:
The WHI study (first arm published in JAMA 2002) was terminated early because the combination of premarin and provera (Prempro) caused increased breast cancer and heart disease. Immediately after this study was published, there was a massive switch by women to bio-identical hormones which resulted in a 4 billion dollar loss for Wyeth, the maker of Prempro. (13)
WHI Study (Second Arm):
All the women in the second arm of the WHI study had prior hysterectomies (uterus absent), so they did not need the synthetic progestin, Provera commonly given to prevent endometrial cancer. Rather, they were only given Premarin (the horse hormone, also called CEE, for Conjugated Equine Estrogen). Unlike the first arm of the study, these women had no increase in breast cancer risk.(18) (see chart below)
Click here for data chart from the second arm of the WHI in JAMA 2004.(14)

Above Chart: Adverse Events in the Second Arm of WHI study: Blue Bars Placebo Group. Red Bars estroegn-only (CEE). Note the above chart shows less heart disease, less breast cancer, less colon cancer, less factures and fewer deaths in the estrogen (CEE) group. Above Chart Courtesy of Susan Ott MD Bone Physiology.(19)
Premarin estrogen (CEE) causes endometrial cancer, so the mainstream medical system always gives Provera (progestins) to prevent endometrial cancer, unless of course, the uterus is absent from prior hysterectomy.(20)
The WHI Culprit was the Synthetic Progestin (an altered form of Progesterone)
Back to the first arm of the WHI which used Prempro, it is clear from the data that the culprit which caused breast cancer and heart disease was Provera (MPA, medroxyprogesterone), a synthetic monster hormone. For years, Provera has been known to cause heart disease and breast cancer.(21-22)(39)
 Monster Hormones are Chemically Altered
Monster Hormones are Chemically Altered
Chemically altered synthetic progestins (Provera, MPA, medroxyprogesterone) was used in the first arm of the 2002 WHI study. Synthetic progestins are also used in birth control pills. routinely handed out by the medical system. These chemically altered hormones are monsters that should never have been FDA approved for marketing to the American people. They should be banned.
Image Left: Another Monster: Boris Karloff from Frankenstein 1931.Courtesy of Wikimedia. public domain.
The Media Says Hormones Cause Cancer and Heart Disease
If bio-identical hormones are so safe, then why do the newspapers say that women’s hormones cause breast cancer and heart disease?(23)
The answer is that the media and the medical profession routinely confuse synthetic chemically altered monster hormones with the bio-identical hormones. The drug companies intentionally create this confusion because they want to hide the fact that synthetic hormones are monsters that should be banned. The drug industry must chemically altered a hormone to obtain a patent. By law, naturally occurring bio-identical hormones cannot be patented, thus protecting profits from competition. Examples of monster synthetic hormones are all progestins, and birth control pills which are never found in nature. These are the monster hormones.
A Listing of a Few Monster Hormones:
Chemically Altered forms of progesterone:
Dienogest, Desogestrel, Drospirenone, Dydrogesterone, Ethisterone, Etonogestrel, Ethynodiol diacetate, Gestodene, Gestonorone, Levonorgestrel, Lynestrenol, Medroxyprogesterone, Megestrol, Norelgestromin, Norethisterone, Norethynodrel, Norgestimate, Norgestrel, Norgestrienone, Tibolone
Chemically altered forms of estrogen:
Dienestrol, Diethylstilbestrol, Ethinylestradiol, Fosfestrol, Mestranol
Chemically alered hormones in BCP’s Birth Control Pills:
levonorgestrel and ethinyl estradiol [oral contraceptive] (ALESSE 28, AVIANE, NORDETTE, SEASONALE, TRIPHASIL, TRIVORA-28); norethindrone and ethinyl estradiol (COMBI PATCH, LOESTRIN FE 1/20, NEOCON 1/35, ORTHO-NOVUM 7/7/7, OVCON 35); norgestimate and ethinyl estradiol (ORTHO-CYCLEN, ORTHOTRI-CYCLEN, TRINESSA); norgestrel and ethinyl estradiol (LO/OVRAL 28, LOW-OGESTREL), desogestrel and ethinyl estradiol (DESOGEN, MIRCETTE, ORTHO-CEPT), drospirenone and ethinyl estradiol (YASMIN)
Chemically altered forms of testosterone:
Androstanolone, Fluoxymesterone, Mesterolone, Methyltestosterone
How to make a Monster Hormone, Add a Side-Chain (in Red below)
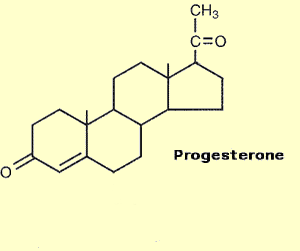

Human Progesterone Medroxyprogesterone (Provera) – the Monster Hormone
Take a good look at human bio-identical Progesterone (Upper Left), and the chemically altered version (upper right) Provera (medroxyprogesterone). The added side-chains are labeled in RED on the right side of the Provera molecule. This side-chains (in red) are added in order to make a totally new chemical structure that can be patented. This creates a monster. In the opinion of John R Lee MD, “to prescribe a chemically altered version of progesterone called Provera is medical malpractice”, and yet this practice is common in mainstream medicine. Above Images: Left Natural Progesterone, Right Synthetic medroxyprogesterone, Courtesy of wikimedia commons.author Rhododendronbusch
High Hormone Levels of Pregnancy Protect from Breast Cancer
 In Italy in 1713, breast cancer was quite rare. An Italian doctor, Bernardino Ramazzini (1633–1714) noted a relatively higher incidence of breast cancer in nuns at the local convent compared to married women, and wondered if this was related to celibate lifestyle. (24)
In Italy in 1713, breast cancer was quite rare. An Italian doctor, Bernardino Ramazzini (1633–1714) noted a relatively higher incidence of breast cancer in nuns at the local convent compared to married women, and wondered if this was related to celibate lifestyle. (24)
In 2005, Dr. Jose Russo studied the role of pregnancy conferring protection from breast cancer, finding single and multiple pregnancies confer protection from breast cancer, while no pregnancies (as in the nun in a convent) leads to increased risk of breast cancer. Dr. Russo writes:
Women who gave birth to a child when they were younger than 24 years of age exhibit a decrease in their lifetime risk of developing breast cancer, and additional pregnancies increase the protection. The protective effect of full-term pregnancy is a well-established concept not only in humans, but also in experimental rodent models. (25)
What is the Molecular Mechanism of Pregnancy Induced Protection from Breast Cancer?
Since pregnancy confers protection from breast cancer, perhaps this holds the key to understanding how to prevent and treat breast cancer.In 2019 and 2020, Dr Mary Feigman studied this question in a transgenic mouse model called CAGMYC. These are mice inbred to have overexpression of the cMYC oncogene. Dr. Mary Feigman found that in this CAGMYC mouse model, pregnancy conferred protection by increasing the P53 protein content in the MECs (mammary epithelial cells) that blocked the development of malignancy. Pregnancy made the MEC’s less responsive to cMYC oncogene overexpression, thus blocking the devopment of premalignant lesions, writing:
But how can pregnancy decrease mammary oncogenesis?…To characterize the influence of a pregnancy-induced epigenome on the response to oncogene expression, we used a transgenic mouse strain (CAGMYC), in which overexpression of the oncogene cMYC, an inducer of mammary tumor development23, is driven in a doxycycline (DOX)-dependent manner…Using this transgenic mouse strain, we found that the post-pregnancy epigenome was incompatible with cMYC overexpression, blocking the activation of MYC-downstream signals and their progression to oncogenesis… Our study revealed a substantial increase of p53 protein in post-pregnancy CAGMYC [transgenic mice with cMYC overexpression] organoids, possibly promoting a senescent state that could block the development of malignant phenotypes…Using inducible cMYC overexpression, we demonstrate that post-pregnancy MECs are resistant to the downstream molecular programs induced by cMYC, a response that blunts carcinoma initiation, but does not perturb the normal pregnancy-induced epigenomic landscape…Using this system, we confirmed post-pregnancy MECs are less responsive to cMYC overexpression. (63-64)
Note: P53 is called “the Guardian of the Genome” because the P53 protein is involved in repairing DNA damage or else induciing cell apoptosis if the damage cannot be repaired, a form of cancer surveillance.
Bioidentical Hormones Prevent Breast Cancer in Mouse Models
This protection from breast cancer is thought to be conferred by high hormones levels of estrogen and progesterone of pregnancy. This was confirmed in 2007 by Dr. Lakshmanaswamy Rajkumar who studied two different models of genetically engineered mice who spontaneously develop breast cancer. When Dr. Rajkumar simulated pregnant hormone states in mice by treating them with estrogen, progesterone and testosterone, the incidence of breast cancer was drastically reduced, demonstrating that hormone treatment protected genetically engineered mice from developing breast cancer. In a third model of breast cancer using human breast cancer cells xenografted in mice, natural, bioidentical hormone treatment again markedly inhibited cancer progression. (26) (65-70)
In 2013, Dr. Arunkumar Arumugam studied a mouse model in which breast cancer is induced by injection of a carcinogenic chemical, N-methyl-N-nitrosourea. Prior to injection of the carcinogen chemical, Dr Arumugam gave the mice short treatment with pregnancy levels of estradiol, finding this very effective in preventing carcinogenesis, writing:
We have earlier demonstrated that short-term treatment with pregnancy levels of estradiol (STET) is very effective in preventing mammary carcinogenesis. Rats were injected with N-methyl-N-nitrosourea at 7 weeks of age and divided into 2 groups. Short-term treatment with pregnancy levels of estradiol drastically reduced the incidence of overt mammary cancers. …The transplantation experiment indicated that the progression of LMMC [latent microscopic mammary cancers] was dependent on the systemic environment it is exposed to. The LMMC derived from control were not able to progress further to make overt cancers when transplanted STET hosts, while the LMMC derived from STET were able to progress to overt cancers when transplanted to control hosts. These findings demonstrate that STET confers protection against mammary cancer development by blocking promotion and progression of transformed cells. (69)
Adding Progesterone Inhibits Estrogen Stimulated Breast Cancer in Mouse Model
In 1985, Dr Akira Inoh from Japan showed progesterone prevented breast cancer in inbred W/Fu strain mice treated with estrogens. These mice were prone to develop spontaneous cancers of various types, including breast cancer. When the mice were ovariectomized and given prolonged treatment with diethylstilbestrol [synthetic estrogen] or 17 beta-estradiol [natural estrogen], the mice developed multiple breast tumors. However, when when the mice were simultaneously given progesterone along with the estrogen, the “multiplicity and size of estrogen-induced MTs [multiple tumors] were reduced by the simultaneous administration of either progesterone or tamoxifen”. Further discussion of progesterone as breast cancer protective can be found in the Safety and Adverse Effects of Progesterone. (70)
Radiation Induced Breast Cancer Prevented with Progesterone
In 1973, Dr. Albert Segaloff from New Orleans studied a mouse model of radiation induced breast cancer. When the mice were pre-treated with progesterone pellets, none of them developed radiation induced breast cancer, writing:
In this preliminary experiment none of the animals that bore just progesterone pellets and were radiated developed mammary carcinomata. (71)
Above left image: M-Mode Ultrasound Image of early pregnancy, Author: Nevit Dilmen, courtesy of Wikimedia commons.
Progesterone Deficiency Increases Risk for Breast Cancer 5.4-Fold
In 1981, Dr. Linda Cowan studied the incidence of breast cancer in women with progesterone deficiency. Dr. Cowan studied 1,083 women evaluated and treated for infertility between 1945 and 1965, then followed through April 1978 to determine the incidence of breast cancer. Women with progesterone deficiency had 5.4 times greater incidence of breast cancer compared to women with infertility due to non-hormonal causes. The women with progesterone deficiency experienced a 10-fold increased mortality from all cancers. Dr. Cowan writes:
These [1,083 progesterone deficient ] women were categorized as to the cause of infertility into two groups, those with endogenous progesterone deficiency (PD) and those with nonhormonal causes (NH). Women in the PD group had 5.4 times the risk of premenopausal breast cancer compared to women in the NH group…Women in the PD group also experienced a 10-fold increase in deaths from all malignant neoplasms compared to the NH group. (27)
Progesterone Induces Apoptosis in Breast Cancer, In Vitro Study
In 1998, Drs. Bent Formby, and T. S. Wiley studed in-vitro the effect of progesterone on T47-D breast cancer cells which have the progesterone receptor, finding a strong anti-proliferative effect. Progesterone at the same concentration as third trimester of pregnancy induced apoptosis in the breast cancer cells with downregulation of the anti-apoptosis protein, bcl-2, and upregulation of the p53 protein, known as the “guardian of the genome”. Dr. Bent Formby writes:
the expression by T47-D cancer cells of bcl-2 was down-regulated, and that of p53 was up-regulated as detected by semiquantitative RT-PCR analysis. These results demonstrate that progesterone at a concentration similar to that seen during the third trimester of pregnancy exhibited a strong antiproliferative effect on at least two breast cancer cell lines. Apoptosis was induced in the progesterone receptor expressing T47-D breast cancer cells.
Natural Progesterone Was the First Birth Control Drug
Initially back in the 1940’s, natural progesterone was as an injectable drug used to inhibit ovulation, and thus explored as contraception. This was before oral micronized progesterone was available, so synthetic progestins were developed to provide an oral version which would be more convenient than the injections. The advantage of synthetic progestins was number one, it is more convenient to take an oral tablet, and the added bonus is the manufacture could obtain patent protection for the altered chemical formula. Natural progesterone can not be patented, since it is a natural substance exempt from patent protection. Birth control pills are effective at preventing pregnancy by suppressing ovulation and shutting down ovarian function. Unfortunately synthetic progestins contained in the birth control pills are carcinogenic and cause breast cancer. The pills have many other adverse side effects such as blood clots and strokes. It is advised one should avoid synthetic progestins, as these are monster hormones. Instead. non-hormonal means of contraception are available such as barrier methods with the diaphragm and cervical cap. The non-hormonal copper T IUD is no longer recommended, in litigation for product defect, with breakage and retention of the plastic arm upon attempted removal. For more on Birth Control Pills see: Adverse Effects of Birth Control Pills Part One and Birth Control Pills, Part Two. (29-31)
More on Breast Cancer and Hormone Levels
If higher estrogen levels are the primary cause of breast cancer, we would expect to find more breast cancer mortality in women with higher hormone levels at age 30, and less breast cancer in women with low hormone levels at age 60 (post-menopausal). What we find is the exact opposite. However, what we find is the exact opposite. Two thirds of the breast cancers are found in post-menopausal women, who have ovarian failure with low hormone levels and only one third in younger pre-menopausal women with regular menstrual cycles with higher hormone levels. In 2001, Dr. Rosemary Yancik writes:
Postmenopausal women aged 55 years and older have 66% of incident breast tumors and experience 77% of breast cancer mortality. (72)
Conclusion: In conclusion, bio-identical hormones used at appropriate dosages are safe, effective, and beneficial for health. They are safest when used in the correct combination, much like a symphony with multiple musical instruments makes beautiful music. On the other hand, any chemical alteration of a human hormone creates a monster. One example is medroxyprogesterone (MPA), a chemically altered version of progesterone used to induce cancer in the MPA mouse model of breast cancer. These monster hormones should never have been FDA approved for marketing and sale to the American people. Synthetic versions of human hormones are unsafe, causing cancer and heart disease, and should be banned immediately.
==================================================================
 Click Here for link to book on Amazon:
Click Here for link to book on Amazon:
Bioidentical Hormones 101 Second Edition (2025) by Jeffrey Dach MD
Three Volume Series e-book. Read the ebook for only 99 cents! Limited Time.
Articles with Related Interest:
Free Video Introduction to Book
Introduction Video to Bioidentical Hormones 101 Second Edition (2025)
Bioidentical Hormones for Breast Cancer Survivors Video Presentation
Articles with Related Interest:
Hormone Replacement for Breast Cancer Survivors Part One
Hormone Replacement for Breast Cancer Survivors Part Two
Estrogen Metabolism, Iodine, 2MEO Part Three
Testosterone for Breast Cancer Prevention and Treatment
All Bioidentical Hormone Articles
Articles With Related Interest
The Safety of Bio-Identical Hormones
The Importance of BioIdentical Hormones
Bioidentical Hormones Prevent Arthritis
Bioidentical Hormone Estrogen Prevents Heart Disease
Morning Rounds With Steven Economou MD
Waking Up from the Synthetic Hormone Nightmare
HRT Does Not Cause Breast Cancer
Inept FDA Declares War on Bioidentical Hormones
Articles on the Safety of BioIdentical Hormones
(1) The Case for Bioidentical Hormones Steven F Hotze MD. 2008.(33)
(2) The Safety of Bioidentical Hormones — the Data vs. the Hype by Jacob Teitelbaum, MD From the Townsend Letter June 2007.(34)
(3) The Truth About Hormone Therapy By Erika Schwartz , Kent Holtorf , and David Brownstein March 16, 2009 WSJ
4) Hormones-in-Wellness and Disease Prevention Holtorf Schwartz By Erika Schwartz and Kent Holtorf
5) Natural_vs_Synthetic_HRT_Literature_Review Kent Holtorf
6) Bioidentical-hormone-debateThe bioidentical hormone debate Holtorf_Kent_Postgraduate medicine_2009
Recommended Reading: books by John R Lee MD (35)
WHAT YOUR DOCTOR MAY NOT TELL YOU ABOUT MENOPAUSE: The Breakthrough Book on Natural Progesterone (Warner Books, 1996)(35)
WHAT YOUR DOCTOR MAY NOT TELL YOU ABOUT PREMENOPAUSE: Balance Your Hormones and Your Life from Thirty to Fifty (Warner Books, 1999)(35)
WHAT YOUR DOCTOR MAY NOT TELL YOU ABOUT BREAST CANCER: How Hormone Balance Can Help Save Your Life, (Warner Books, 2002)(35)
Jeffrey Dach MD
7450 Griffin Road Suite 190
Davie Fl 33314
954-792-4663
www.naturalmedicine101.com
www.truemedmd.com
References
1) Farrell, D. J., and L. Bower. “Fatal water intoxication.” Journal of clinical pathology 56.10 (2003): 803-804.
2) Stack, David. “Charles Darwin: theory of natural selection.” Encyclopedia of Evolutionary Psychological Science. Cham: Springer International Publishing, 2021. 1000-1011.
(3) http://www.johnleemd.com/store/premenstrual_syndrome.html
Excerpted From: WHAT YOUR DOCTOR MAY NOT TELL YOU ABOUT BREAST CANCER:
Balance Your Hormones and Your Life from Thirty to Fifty. PHYSIOLOGICAL EFFECTS OF ESTROGEN AND PROGESTERONE. How Hormone Balance Can Help Save Your Life. by John R. Lee, M.D., David Zava, Ph.D. and Virginia Hopkins. Warner Books 2002
4) Natural Hormone Balance for Women: Look Younger, Feel Stronger, and Live Life with Exuberance. by Uzzi Reiss MD
5) Wolfe, M. Michael, David R. Lichtenstein, and Gurkirpal Singh. “Gastrointestinal toxicity of nonsteroidal antiinflammatory drugs.” New England Journal of Medicine 340.24 (1999): 1888-1899.
6) FDA Press COnference on Bioidentical Hormones Jan 2008
Transcript of FDA Press Conference on FDA Actions on Bio-Identical Hormones
FTS HHS FDA Susan Cruzan January 9, 2008
7) deleted
8A) Fournier A, Berrino F, Clavel-Chapelon F. Unequal risks for breast cancer associated
with different hormone replacement therapies: results from the E3N cohort study. Breast Cancer Res Treat 2008;107:103–11
8B) Fournier A, Berrino F, Riboli E, et al. Breast cancer risk in relation to different types
of hormone replacement therapy in the E3N-EPIC cohort. Int J Cancer 2005; 114:448–54.
8C) De Lignieres, B., et al. “Combined hormone replacement therapy and risk of breast cancer in a French cohort study of 3175 women.” Climacteric 5.4 (2002): 332-340.
(9) http://www.johnleemd.com/store/cancer_progest.html
Breast Cancer Book Intro. WHAT YOUR DOCTOR MAY NOT TELL YOU ABOUT BREAST CANCER. How Hormone Balance Can Help Save Your Life
By John R. Lee, M.D., David Zava Ph.D., and Virginia Hopkins INTRODUCTION
(10) Breast Cancer Prevention and Iodine Supplementation by Jeffrey Dach MD
(11) http://content.nejm.org/cgi/content/short/356/25/2591
Estrogen Therapy and Coronary-Artery Calcification. NEJM Volume 356:2591-2602 June 21, 2007 Number 25. JoAnn E. Manson, M.D., et al.
(12) http://www.ncbi.nlm.nih.gov/pubmed/15989413
J Womens Health (Larchmt). 2005 Jun;14(5):410-7. Effects of hormone replacement on progression of coronary calcium as measured by electron beam tomography.Budoff MJ, et al.
(13) http://jama.ama-assn.org/cgi/content/abstract/288/3/321
Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women
Principal Results From the Women’s Health Initiative Randomized Controlled Trial
Writing Group for the Women’s Health Initiative Investigators JAMA. 2002;288:321-333. First Arm.
(14) http://jama.ama-assn.org/cgi/content/full/291/14/1701
Effects of Conjugated Equine Estrogen in Postmenopausal Women With Hysterectomy
The Women’s Health Initiative Randomized Controlled Trial. JAMA. 2004;291:1701-1712. Second Arm. This is the Second Arm of the Study. Premarin Only.
(15) http://en.wikipedia.org/wiki/Premarin
Premarin From Wikipedia, the free encyclopedia
(16) http://en.wikipedia.org/wiki/Medroxyprogesterone
Provera, Medroxyprogesterone, From Wikipedia, the free encyclopedia
(17) http://homecoalition.org/TakeAction
Take Action. Write a letter to your elected officials using our online advocacy tool.
Act now to defend your right to bio-identical hormones! Please contact your
congressional representative, senators, and the White House immediately.
HOMECoalition.org.
(18) http://jama.ama-assn.org/cgi/content/full/295/14/1647
Effects of Conjugated Equine Estrogens on Breast Cancer and Mammography Screening in Postmenopausal Women With Hysterectomy. Marcia L. Stefanick, PhD et al. for the WHI Investigators. JAMA. 2006;295:1647-1657. Conclusions Treatment with CEE alone for 7.1 years does not increase breast cancer incidence in postmenopausal women with prior hysterectomy.
(19)
http://courses.washington.edu/bonephys/opestrogen.html#WHI
Osteoporosis and Bone Physiology, Susan Ott, MD, Associate Professor, Department of Medicine, University of Washington. A Review of the results from the Women’s Health Initiative.
20) Key, T. J. A., and M. C. Pike. “The dose-effect relationship between ‘unopposed’oestrogens and endometrial mitotic rate: its central role in explaining and predicting endometrial cancer risk.” British journal of cancer 57.2 (1988): 205-212.
(21) http://atvb.ahajournals.org/cgi/content/full/24/7/1171
Should Progestins Be Blamed for the Failure of Hormone Replacement Therapy to Reduce Cardiovascular Events in Randomized Controlled Trials?
Kwang Kon Koh; Ichiro Sakuma. Arteriosclerosis, Thrombosis, and Vascular Biology. 2004;24:1171.
(22) http://www.ncbi.nlm.nih.gov/pubmed/16841178
Effects of estradiol with micronized progesterone or medroxyprogesterone acetate on risk markers for breast cancer in postmenopausal monkeys.Wood CE et al. Breast Cancer Res Treat. 2007 Jan;101(2):125-34.
23)The Truth About Hormones Monday, Jul. 22, 2002 Time Magazine. By CHRISTINE GORMAN AND ALICE PARK
(24) Lukong, Kiven Erique. “Understanding breast cancer–The long and winding road.” BBA clinical 7 (2017): 64-77.
25) Russo, Jose, et al. “The protective role of pregnancy in breast cancer.” Breast cancer research 7 (2005): 1-12.
Women who gave birth to a child when they were younger than 24 years of age exhibit a decrease in their lifetime risk of developing breast cancer, and additional pregnancies increase the protection [3]. The protective effect of full-term pregnancy is a well-established concept not only in humans, but also in experimental rodent models [4-12].
26) Rajkumar, Lakshmanaswamy, et al. “Hormone-induced protection of mammary tumorigenesis in genetically engineered mouse models.” Breast Cancer Research 9 (2007): 1-11.
27) Cowan, Linda D., et al. “Breast cancer incidence in women with a history of progesterone deficiency.” American Journal of Epidemiology 114.2 (1981): 209-217.
In order to investigate the nature of the association of involuntarily delayed first birth and risk of breast cancer, 1083 white women who had been evaluated and treated for infertility from 1945–1965 were followed prospectively through April 1978 to ascertain their breast cancer incidence. These women were categorized as to the cause of infertility into two groups, those with endogenous progesterone deficiency (PD) and those with nonhormonal causes (NH). Women in the PD group had 5.4 times the risk of premenopausal breast cancer compared to women in the NH group. This excess risk could not be explained by differences between the two groups in ages at menarche or menopause, history of oral contraceptive use, history of benign breast dis ease or age at first birth. Women in the PD group also experienced a 10-fold increase in deaths from all malignant neopiasms compared to the NH group. The Incidence of postmenopausal breast cancer did not differ significantly between the two groups
28) Formby, Bent, and T. S. Wiley. “Progesterone inhibits growth and induces apoptosis in breast cancer cells: inverse effects on Bcl-2 and p53.” Annals of Clinical & Laboratory Science 28.6 (1998): 360-369.
Progesterone inhibits the proliferation of normal breast epithelial cells in vivo, as well as breast cancer cells in vitro. But the biologic mechanism of this inhibition remains to be determined. We explored the possibility that an antiproliferative activity of progesterone in breast cancer cell lines is due to its ability to induce apoptosis. Since p53 and bcl-2 genetically control the apoptotic process, we investigated whether or not these genes could be involved in the progesterone-induced apoptosis. We found a maximal 90 percent inhibition of cell proliferation with T47-D breast cancer cells after exposure to 10 microM progesterone for 72 hours. Control progesterone receptor negative MDA-231 cancer cells were unresponsive to these two concentrations of progesterone. After 24 hours of exposure to 10 microM progesterone, cytofluorometric analysis of T47-D breast cancer cells demonstrated 43 percent had undergone apoptosis without signs of necrosis. After 72 hours of exposure to 10 microM progesterone, 48 percent of the cells had undergone apoptosis and 40 percent demonstrated “leaky” membranes. Untreated cancer cells did not undergo apoptosis. Evidence proving apoptosis was also demonstrated by fragmentation of nuclear DNA into multiples of oligonucleosomal fragments. After 24 hours of exposure to either 1 microM or 10 microM progesterone, the expression by T47-D cancer cells of bcl-2 was down-regulated, and that of p53 was up-regulated as detected by semiquantitative RT-PCR analysis. These results demonstrate that progesterone at a concentration similar to that seen during the third trimester of pregnancy exhibited a strong antiproliferative effect on at least two breast cancer cell lines. Apoptosis was induced in the progesterone receptor expressing T47-D breast cancer cells.
(29) http://en.wikipedia.org/wiki/Birth_control_pill
Combined oral contraceptive pill. From Wikipedia, the free encyclopedia. (Redirected from Birth control pill)
(30) http://www.worstpills.org/results.cfm?disease_id=26
Oral Contraceptives on Worst Pills.org. The pill can cause many adverse effects. Some of them are merely a nuisance, while others can be life-threatening. The pill can cause headaches, bloating, nausea, irregular bleeding and spotting, breast tenderness, weight gain, or vision changes. Other more serious adverse effects that can occur from a few months to a few years after starting oral contraceptives include high blood pressure, gallbladder disease, liver tumors, depression, and metabolic disorders, such as diabetes. Temporary infertility has been associated with the period of time right after pill use is stopped. But the two most dangerous risks associated with taking birth control pills are blood clots and cancer.
(31)
http://www.jeffreywarber.com/hc%20pages/pillsideeffects.html
Birth Control Pill Adverse Side Effects by Jeffrey Warber MD
(32) http://www.quickoverview.com/reproductive/birth-control-pill.html
History and Development of an effective combined oral contraceptive. People Involved.
(33) http://www.jpands.org/vol13no2/hotze.pdf
Point/Counterpoint: The Case for Bioidentical Hormones Steven F. Hotze, M.D.Donald P. Ellsworth, M.D.Journal of American Physicians and Surgeons Volume 13 Number 2 Summer 2008
(34)
http://www.townsendletter.com/June2007/painfree0607.htm
The Safety of Bioidentical Hormones — the Data vs. the Hype by Jacob Teitelbaum, MD
(35) http://www.johnleemd.com/store/main_books.html
Books by John R Lee MD
Wyeth and the FDA
(36) http//:naturalnews.com/022595.html
FDA’s Assault of Bioidentical Hormones Demonstrates Pro-Pharma Loyalties, Disregard for Consumer Choice Tuesday, February 05, 2008 by: Mike Adams
(37) February 16, 2008. Women, Doctors Wage Crucial Battle With FDA To Save Bioidentical Hormones From Wyeth’s Wrath. A major coalition of informed women and their doctors have launched an all out war on the Federal Drug Administration’s (FDA) cynical and corrupt decision to ban compounded hormones containing Estriol.
(38) FDA Declares War on BioIdentical Hormones by Jeffrey Dach MD
Provera and Heart Disease
(39) http://atvb.ahajournals.org/cgi/content/full/17/1/217
Medroxyprogesterone Acetate Antagonizes Inhibitory Effects of Conjugated Equine Estrogens on Coronary Artery Atherosclerosis. Michael R. Adams; Thomas C. Register; Deborah L. Golden; Janice D. Wagner; J. Koudy Williams .Arteriosclerosis, Thrombosis, and Vascular Biology. 1997;17:217-221.
41) Giulianelli, Sebastián, et al. “Estrogen receptor alpha mediates progestin-induced mammary tumor growth by interacting with progesterone receptors at the cyclin D1/MYC promoters.” Cancer research 72.9 (2012): 2416-2427.
42) Dhanasekaran, Renumathy, et al. “The MYC oncogene—the grand orchestrator of cancer growth and immune evasion.” Nature reviews Clinical oncology 19.1 (2022): 23-36.
43) Kim, Jong Kyong, and J. Alan Diehl. “Nuclear cyclin D1: an oncogenic driver in human cancer.” Journal of cellular physiology 220.2 (2009): 292-296.
44) Perkins, Meghan S., et al. “Upregulation of an estrogen receptor-regulated gene by first generation progestins requires both the progesterone receptor and estrogen receptor alpha.” Frontiers in Endocrinology 13 (2022): 959396.
45) de Lignières B. Effects of progestogens on the postmenopausal breast. Climacteric
2002;5:229–35.
46) Campagnoli C, Clavel-Chapelon F, Kaaks R, et al. Progestins and progesterone in
hormone replacement therapy and the risk of breast cancer. J Steroid Biochem Mol
Biol 2005;96:95–108.
47) Ory K, Lebeau J, Levalois C, et al. Apoptosis inhibition mediated by medroxyprogesterone acetate treatment of breast cancer cell lines. Breast Cancer Res Treat 2001;68:187–98. 554
48) Hofseth LJ, Raafat AM, Osuch JR, et al. Hormone replacement therapy with estrogen or estrogen plus medroxyprogesterone acetate is associated with increased epithelial proliferation in the normal postmenopausal breast. J Clin Endocrinol Metab 1999;84:4559–65.
49) Jeng MH, Parker CJ, Jordan VC. Estrogenic potential of progestins in oral contraceptives stimulate human breast cancer cell proliferation. Cancer Res 1992;52:6539–46.
50) Kalkhoven E, Kwakkenbos-Isbrücker L, de Laat SW, et al. Synthetic progestins induce proliferation of breast tumor cell lines via the progesterone or estrogen receptor. Mol Cell Endocrinol 1994;102:45–52.
51) Papa V, Reese CC, Brunetti, et al. Progestins increase insulin receptor content and insulin stimulation of growth in human breast carcinoma cells. Cancer Res 1990;50:7858–62.
52) Hissom JR, Moore MR. Progestin effects on growth in the human breast cancer cell
line T-47D—possible therapeutic implications. Biochem Biophys Res Commun 1987;145:706–11.
53) Catherino H,Jeng MH, Jordan VC. Norgestrel and gestodene stimulate breast cancer
cell growth through an oestrogen receptor mediated mechanism. Br J Cancer 1993;67:
945–52.
54) Cline JM, Soderqvist G, von Schoultz E, et al. Effects of conjugated estrogens,
medroxyprogesterone acetate, and tamoxifen on the mammary glands of macaques. Breast Cancer Res Treat 1998;48:221–9
55) Berkson, D. Lindsey. Hormone Deception. Contemporary Books., 2000.
56) Colborn, Theo, Dianne Dumanoski, and John Peterson Myers. Our stolen future: Are we threatening our fertility, intelligence, and survival?–a scientific detective story. Penguin, 1997.
57) Escrich, Edward. “Validity of the DMBA-induced mammary cancer model for the study of human breast cancer.” The International journal of biological markers 2.3 (1987): 197-206.
58) Buqué, Aitziber, et al. “MPA/DMBA-driven mammary carcinomas.” Methods in cell biology. Vol. 163. Academic Press, 2021. 1-19.
59) Lanari, Claudia Lee Malvina, et al. “The MPA mouse breast cancer model: evidence for a role of progesterone receptors in breast cancer.” (2009).
60) Cavalieri, Ercole, and Eleanor Rogan. “The 3, 4-quinones of estrone and estradiol are the initiators of cancer whereas resveratrol and N-acetylcysteine are the preventers.” International journal of molecular sciences 22.15 (2021): 8238.
61) Cavalieri, Ercole L., and Eleanor G. Rogan. “Inhibition of depurinating estrogen-DNA adduct formation in the prevention of breast and other cancers.” Trends in breast cancer prevention (2016): 113-145.
62) Cavalieri, Ercole L., and Eleanor G. Rogan. “The etiology and prevention of breast cancer.” Drug Discovery Today: Disease Mechanisms 9.1-2 (2012): e55-e69.
63) Feigman, Mary J., et al. “Pregnancy reprograms the epigenome of mammary epithelial cells and blocks the development of premalignant lesions.” Nature communications 11.1 (2020): 2649.
But how can pregnancy decrease mammary oncogenesis?…To characterize the influence of a pregnancy-induced epigenome on the response to oncogene expression, we used a transgenic mouse strain (CAGMYC), in which overexpression of the oncogene cMYC, an inducer of mammary tumor development23, is driven in a doxycycline (DOX)-dependent manner… Our study revealed a substantial increase of p53 protein in post-pregnancy CAGMYC [transgenic mice] organoids, possibly promoting a senescent state that could block the development of malignant phenotypes.
Using inducible cMYC overexpression, we demonstrate that post-pregnancy MECs are resistant to the downstream molecular programs induced by cMYC, a response that blunts carcinoma initiation, but does not perturb the normal pregnancy-induced epigenomic landscape. cMYC overexpression drives post-pregnancy MECs into a senescence-like state, and perturbations of this state increase malignant phenotypic changes.
Importantly, our mammary organoid experiments confirmed the cell-autonomous characteristics of pregnancy-induced changes, and their ability to block responses to cMYC overexpression. Using this system, we confirmed post-pregnancy MECs are less responsive to cMYC overexpression.
64) Feigman, Mary J., et al. “Pregnancy reprograms the enhancer landscape of mammary epithelial cells and alters the response to cMYC-driven oncogenesis.” bioRxiv (2019): 642330.
transgenic mouse strain (CAGMYC), in which overexpression of the oncogene cMYC, a known inducer of mammary tumor development [7, 23, 24], is driven in a doxycycline-dependent manner. Using this transgenic mouse strain, we found that the post-pregnancy epigenome was incompatible with cMYC overexpression, blocking the activation of MYC-downstream signals and their progression to oncogenesis.
65) Rajkumar, Lakshmanaswamy, et al. “Short-term exposure to pregnancy levels of estrogen prevents mammary carcinogenesis.” Proceedings of the National Academy of Sciences 98.20 (2001): 11755-11759.
66) Rajkumar, Lakshmanaswamy, et al. “Prevention of mammary carcinogenesis by short-term estrogen and progestin treatments.” Breast Cancer Research 6.1 (2003): 1-7.
67) Rajkumar, Lakshmanaswamy, et al. “Hormone-induced protection of mammary tumorigenesis in genetically engineered mouse models.” Breast Cancer Research 9 (2007): 1-11.
68) Lakshmanaswamy, Rajkumar, Raphael C. Guzman, and Satyabrata Nandi. “Hormonal prevention of breast cancer: significance of promotional environment.” Hormonal Carcinogenesis V. New York, NY: Springer New York, 2008. 469-475.
69) Arumugam, Arunkumar, et al. “Short-term treatment with pregnancy levels of estradiol prevents breast cancer by delaying promotion and progression.” Cancer Research 73.8_Supplement (2013): 199-199.
We have earlier demonstrated that short-term treatment with pregnancy levels of estradiol (STET) is very effective in preventing mammary carcinogenesis. Rats were injected with N-methyl-N-nitrosourea at 7 weeks of age and divided into 2 groups. Short-term treatment with pregnancy levels of estradiol drastically reduced the incidence of overt mammary cancers. …The transplantation experiment indicated that the progression of LMMC [latent microscopic mammary cancers] was dependent on the systemic environment it is exposed to. The LMMC derived from control were not able to progress further to make overt cancers when transplanted STET hosts, while the LMMC derived from STET were able to progress to overt cancers when transplanted to control hosts. These findings demonstrate that STET confers protection against mammary cancer development by blocking promotion and progression of transformed cells.
70) Arumugam, Arunkumar, Elaine A. Lissner, and Rajkumar Lakshmanaswamy. “The role of hormones and aromatase inhibitors on breast tumor growth and general health in a postmenopausal mouse model.” Reproductive Biology and Endocrinology 12 (2014): 1-13.
————————– –
70) Inoh, Akira, et al. “Protective effects of progesterone and tamoxifen in estrogen-induced mammary carcinogenesis in ovariectomized W/Fu rats.” Japanese Journal of Cancer Research GANN 76.8 (1985): 699-704.
71) Segaloff, Albert. “Inhibition by progesterone of radiation-estrogen-induced mammary cancer in the rat.” Cancer Research 33.5 (1973): 1136-1137.
72) Yancik, Rosemary, et al. “Effect of age and comorbidity in postmenopausal breast cancer patients aged 55 years and older.” Jama 285.7 (2001): 885-892.
Postmenopausal women aged 55 years and older have 66% of incident breast tumors and experience 77% of breast cancer mortality,
73) Mohammed, Hisham, et al. “Progesterone receptor modulates ERα action in breast cancer.” Nature 523.7560 (2015): 313-317.
====================================== =
74) Gompel, A., Prior, J.C. et al. “Lack of evidence that progesterone in ovulatory cycles causes breast cancer.” Climacteric 26.6 (2023): 634-637.
the breast cancer results from an 8-year prospective observational study with more than 80,000 participants (in France called E3N cohort) which allowed a comparison of breast cancer risk on various single and combined menopausal hormonal therapies (MHT) [22]. This study documented
breast cancer risk in untreated postmenopausal women as controls versus those taking MHT with estradiol alone (risk ratio 1.29, 95% confidence interval 1.02, 1.65) versus estradiol plus progesterone (risk ratio 1.00, 95% confidence interval 0.83, 1.22). Although there was no increased breast cancer risk with estradiol–progesterone, estradiol with synthetic progestin MHT was related to significantly increased risk (risk ratio 1.69, 95% confidence interval 1.50, 1.91) [22]. A recent review summarizes publications on a lower breast cancer risk in MHT of estradiol with micronized progesterone and dydrogesterone versus other progestins [23].
74) Hipolito Rodrigues, Marcio Alexandre, and Anne Gompel. “Micronized progesterone, progestins, and menopause hormone therapy.” Women & Health 61.1 (2021): 3-14.
75) Coelingh Bennink, Herjan JT, et al. “Progesterone from ovulatory menstrual cycles is an important cause of breast cancer.” Breast cancer research 25.1 (2023): 60.
76) Coelingh Bennink, H. J. T., and F. Z. Stanczyk. “Progesterone and not estrogens or androgens causes breast cancer.” Climacteric 27.2 (2024): 217-222.
===========================================
77) Lyytinen, Heli, Eero Pukkala, and Olavi Ylikorkala. “Breast cancer risk in postmenopausal women using estrogen-only therapy.” Obstetrics & Gynecology 108.6 (2006): 1354-1360.
OBJECTIVE: To evaluate whether the risk of estrogen-only therapy on breast cancer varies by dose, constituent,and route of administration.
METHODS: All Finnish women older than age 50 years using oral or transdermal estradiol (n 84,729), oral estriol (n 7,941), or vaginal estrogens (n 18,314) for at least 6 months during 1994 –2001 were identified from the national medical reimbursement register. They were followed for breast cancer with the aid of the Finnish Cancer Registry to the end of 2002.
RESULTS: Altogether, 2,171 women with breast cancer were identified. The standardized incidence ratio of breast cancer with systemic estradiol for less than 5 years was 0.93 (95% confidence interval 0.80 –1.04), and for estradiol use for 5 years or more, 1.44 (1.29 –1.59).
Oral and transdermal estradiol was accompanied by a similar risk of breast cancer. The risk was most prominent with the dose greater than 1.9 mg/d orally; whereas the risk associated with transdermal route was not dose-dependent. The standardized incidence ratio for the lobular type of breast cancer (1.58) was slightly higher than that for the ductal type (1.36). The use of estradiol was associated with both localized breast cancer (1.45; 1.26 –1.66) and cancer spread to regional nodes (1.35; 1.09 –1.65). The incidence of carcinoma in situ (n 32) was increased (2.43; 1.66 –3.42) among estradiol users
CONCLUSION: Estradiol for 5 years or more, either orally or transdermally, means 2–3 extra cases of breast cancer per 1,000 women who are followed for 10 years. Oral estradiol use for less than 5 years, oral estriol, or vaginal estrogens were not associated with a risk of breast cancer.
78) Bakken, Kjersti, et al. “Menopausal hormone therapy and breast cancer risk: impact of different treatments. The European Prospective Investigation into Cancer and Nutrition.” International journal of cancer 128.1 (2011): 144-156.
The EPIC-cohort is a multicentre prospective cohort with 23 contributing centres in 10 European countries [Denmark (Aarhus, Copenhagen), France, Germany (Heidelberg, Potsdam), Great Britain (Cambridge, Oxford), Greece, Italy (Florence, Varese, Ragusa, Turin, Naples), Norway, Spain (Asturias, Granada, Murcia, Navarra, San Sebastian), Sweden (Malmø, Umeå) and The Netherlands (Bilthoven, Utrecht)], covering more than half a million participants.
Menopausal hormone therapy (MHT) is characterized by use of different constituents, regimens and routes of administration.
We investigated the association between the use of different types of MHT and breast cancer risk in the EPIC cohort study. The analysis is based on data from 133,744 postmenopausal women. Approximately 133,744 postmenopausal women contributed to this analysis. Information on MHT was derived from country-specific self-administered questionnaires with a single baseline assessment. Incident breast cancers were identified through population cancer registries or by active follow-up (mean: 8.6 yr). Overall relative risks (RR) and 95% confidence interval (CI) were derived from country-specific Cox proportional hazard models estimates. A total of 4312 primary breast cancers were diagnosed during 1,153,747 person-years of follow-up.
Compared with MHT never users, breast cancer risk was higher among current users of estrogen only (RR: 1.42, 95% CI 1.23–1.64)
and higher still among current users of combined MHT (RR: 1.77, 95% CI 1.40–2.24; p 5 0.02 for combined vs. estrogen-only). Continuous combined regimens conferred a 43% (95% CI: 19–72%) greater risk compared with sequential regimens. There was no significant difference between progesterone and testosterone derivatives in sequential regimens. There was no significant variation in risk linked to the estrogenic component of MHT, neither for oral vs. cutaneous administration nor for estradiol compounds vs. conjugated equine estrogens. Estrogen-only and combined MHT uses were associated with increased breast cancer risk. Continuous combined preparations were associated with the highest risk. Further studies are needed to disentangle the effects of the regimen and the progestin component.
79) Chlebowski, Rowan T., et al. “Randomized trials of estrogen-alone and breast cancer incidence: a meta-analysis.” Breast Cancer Research and Treatment (2024): 1-8.
In the Women’s Health initiative (WHI) randomized clinical trial, conjugated equine estrogen (CEE)-alone significantly reduced breast cancer incidence (P = 0.005). As cohort studies had opposite findings, other randomized clinical trials were identified to conduct a meta-analysis of estrogen-alone influence on breast cancer incidence.
Methods: We conducted literature searches on randomized trials and: estrogen, hormone therapy, and breast cancer, and searches from a prior meta-analysis and reviews. In the meta-analysis, for trials with published relative risks (RR) and 95% confidence intervals (CI), each log-RR was multiplied by weight = 1/V, where V = variance of the log-RR, and V was derived from the corresponding 95% CI. For smaller trials with only breast cancer numbers, the corresponding log-RR = (O – E)/weight, where O is the observed case number in the oestrogen-alone group and E the corresponding expected case number, E = nP.
Results
Findings from 10 randomized trials included 14,282 participants and 591 incident breast cancers. In 9 smaller trials, with 1.2% (24 of 2029) vs 2.2% (33 of 1514) randomized to estrogen-alone vs placebo (open label, one trial) (RR 0.65 95% CI 0.38–1.11, P = 0.12). For 5 trials evaluating estradiol formulations, RR = 0.63 95% CI 0.34–1.16, P = 0.15.
Findings from 10 randomized trials included 14,282 participants and 591 incident breast cancers….Combining the 10 trials, 3.6% (262 of 7339) vs 4.7% (329 of 6943) randomized to estrogen-alone vs placebo (overall RR 0.77 95% CI 0.65–0.91, P = 0.002). Conclusion: The totality of randomized clinical trial evidence supports a conclusion that estrogen-alone use significantly reduces breast cancer incidence.
—————————————
80) Lindberg, Bo S., Bo A. Nilsson, and Elof DB Johansson. “Plasma progesterone levels in normal and abnormal pregnancies.” Acta obstetricia et gynecologica Scandinavica 53.4 (1974): 329-335.
81) Johansson, Elof DB. “Progesterone levels in peripheral plasma during the luteal phase of the normal human menstrual cycle measured by a rapid competitive protein binding technique.” European Journal of Endocrinology 61.4 (1969): 592-606.
82) Holmdahl, Tore H: son, and Elof DB Johansson. “Peripheral plasma levels of 17α-hydroxyprogesterone, progesterone and oestradiol during normal menstrual cycles in women.” European Journal of Endocrinology 71.4 (1972): 743-754.
83) Sandru, Florica, et al. “Progesterone Hypersensitivity in Assisted Reproductive Technologies: Implications for Safety and Efficacy.” Journal of Personalized Medicine 14.1 (2024): 79.
84) Sashidhar, Nivedita, Venkataram Mysore, and G. V. Thejavathy. “Exogenous Progestogen Hypersensitivity and its Increasing Association with Assisted Reproductive Techniques (ART)/in vitro Fertilization (IVF).” Indian Dermatology Online Journal 15.1 (2024): 24-32.
85) Foer, Dinah, et al. “Progestogen hypersensitivity in 24 cases: diagnosis, management, and proposed renaming and classification.” The Journal of Allergy and Clinical Immunology: In Practice 4.4 (2016): 723-729.
86) Lipman, Zoe M., et al. “Autoimmune progesterone dermatitis: a systematic review.” Dermatitis 33.4 (2022): 249-256.
87) Ochnik, Aleksandra M., et al. “Antiandrogenic actions of medroxyprogesterone acetate on epithelial cells within normal human breast tissues cultured ex vivo.” Menopause (New York, NY) 21.1 (2014): 79-88.
In a subset of postmenopausal women, MPA exerts an antiandrogenic effect on breast epithelial cells that is associated with increased proliferation and destabilization of AR protein. This activity may contribute mechanistically to the increased risk of breast cancer in women taking MPA-containing EPT.
Objective: Medroxyprogesterone acetate (MPA), a component of combined estrogen-progestin therapy (EPT), has been associated with increased breast cancer risk in EPT users. MPA can bind to the androgen receptor (AR), and AR signaling inhibits cell growth in breast tissues. Therefore, the aim of this study was to investigate the potential of MPA to disrupt AR signaling in an ex vivo culture model of normal human breast tissue.
Methods: Histologically normal breast tissues from women undergoing breast surgical operation were cultured in the presence or in the absence of the native AR ligand 5α-dihydrotestosterone (DHT), MPA, or the AR antagonist bicalutamide. Ki67, bromodeoxyuridine, B-cell CLL/lymphoma 2 (BCL2), AR, estrogen receptor α, and progesterone receptor were detected by immunohistochemistry.
Results: DHT inhibited the proliferation of breast epithelial cells in an AR-dependent manner within tissues from postmenopausal women, and MPA significantly antagonized this androgenic effect. These hormonal responses were not commonly observed in cultured tissues from premenopausal women. In tissues from postmenopausal women, DHT either induced or repressed BCL2 expression, and the antiandrogenic effect of MPA on BCL2 was variable. MPA significantly opposed the positive effect of DHT on AR stabilization, but these hormones had no significant effect on estrogen receptor α or progesterone receptor levels.
Conclusions: In a subset of postmenopausal women, MPA exerts an antiandrogenic effect on breast epithelial cells that is associated with increased proliferation and destabilization of AR protein. This activity may contribute mechanistically to the increased risk of breast cancer in women taking MPA-containing EPT.
88) Jones, Michael E., et al. “Menopausal hormone therapy and breast cancer: what is the true size of the increased risk?.” British journal of cancer 115.5 (2016): 607-615.
UK Generations Study cohort
The most frequently used serial regimens in our study were Prempak-C (conjugated oestrogen, 625 μg and 1.25 mg; norgestrel, 150 μg), Elleste Duet (estradiol, 1 and 2 mg; norethisterone, 1 mg), and Climagest (Estradiol, 2 mg; norethisterone, 1 mg), and the most frequently used continuous regimens were Premique (conjugated oestrogen, 625 μg; medroxyprogesterone acetate, 5 mg), Kilovance (estradiol, 1 mg; norethisterone, 500 μg), and Kilofem (estradiol, 2 mg; norethisterone, 1 mg).
The HR for oestrogen-only MHT was not increased (HR=1.00; 95% CI: 0.66–1.54).
Among women recruited in 2003–2009, at 6 years of follow-up, 58 148 had reached menopause and 96% had completed a follow-up questionnaire. Among 39 183 women with known menopausal age, 775 developed breast cancer, and the HR in relation to current oestrogen plus progestogen MHT use (based on 52 current oestrogen plus progestogen MHT users in breast cancer cases) relative to those with no previous MHT use was 2.74 (95% confidence interval (CI): 2.05–3.65) for a median duration of 5.4 years of current use, reaching 3.27 (95% CI: 1.53–6.99) at 15+ years of use.
89) Gore, Andrea C., et al. “Introduction to endocrine disrupting chemicals (EDCs).” A guide for public interest organizations and policy-makers (2014): 21-22.
90) Kahn, Linda G., et al. “Endocrine-disrupting chemicals: implications for human health.” The lancet Diabetes & endocrinology 8.8 (2020): 703-718.
91) Hansel, Megan C., et al. “Exposure to Synthetic Endocrine-Disrupting Chemicals in Relation to Maternal and Fetal Sex Steroid Hormones: A Scoping Review.” Current Environmental Health Reports (2024): 1-24.
92) Kek, Tina, Ksenija Geršak, and Irma Virant-Klun. “Exposure to endocrine disrupting chemicals (bisphenols, parabens, and triclosan) and their associations with preterm birth in humans.” Reproductive Toxicology (2024): 108580.
93) Pan, Jing, et al. “The adverse role of endocrine disrupting chemicals in the reproductive system.” Frontiers in Endocrinology 14 (2024): 1324993.
94) Liu, Xiaohui, et al. “Bisphenol-C is the strongest bifunctional ERα-agonist and ERβ-antagonist due to magnified halogen bonding.” PloS one 16.2 (2021): e0246583.
Additional References
Natural_vs_Synthetic_HRT_Literature_Review Holtorf
Bioidentical vs. Synthetic HRT, A review of the literature
The bioidentical hormone debate Holtorf_Kent_Postgraduate medicine_2009: Natural (Bio-Identical) vs. Synthetic HRT by Kent Holtorf, M.D. Dr. Holtorf is the Medical Director of the Holtorf Medical Group, Inc,
http://www.thorne.com/media/hormones11-3.pdf
A Comprehensive Review of the Safety and Efficacy of Bioidentical Hormones for the Management of Menopause and Related Health Risks Deborah Moskowitz, ND. Altern Med Rev 2006;11(3):208-223)
http://www.medscape.com/viewarticle/408096_print
Special Article: Addressing Postmenopausal Estrogen Deficiency: A Position Paper of the American Council on Science and Health January 26, 2001 Sander Shapiro, MD Medscape General Medicine 3(1), 2001.
http://www.womeninbalance.org/research/
research available women in balance.
Fatal Water Intoxication
http://www.msnbc.msn.com/id/16614865/
Woman dies after water-drinking contest
Natural and Synthetic Substances in Medicine
The Promise and Problems of Natural Substances in Medicine Stephen L. DeFelice, M.D.
http://www.iupac.org/publications/pac/2002/pdf/7410×1957.pdf
Natural and synthetic substances related to human health. The dubious honor of being the most powerful toxic substance goes to a protein produced by the bacterium, Clostridium botulinum. This protein is responsible for fatal food poisoning—botulism—being produced when the bacterium grows in the absence of oxygen in canned or preserved food. 2002 IUPAC, Pure and Applied Chemistry 74, 1957–1985
Synthetic Hormones and Breast Cancer
http://www.nwhn.org/healthinfo/detail.cfm?info_id=9&topic=Fact%20Sheets
Menopause Hormone Therapy and Breast Cancer. National Women’s Health Network
http://www.bmj.com/cgi/content/full/310/6979/598/b
BMJ 1995;310:598 (4 March) Letters Risk factors for breast cancer
Hormone Levels, Age and Breast Cancer
http://www.cdc.gov/cancer/breast/statistics/age.htm
Risk of Breast Cancer by Age, CDC .Percent of U.S. Women Who Die from Breast Cancer Over 10-, 20-, and 30-Year Intervals. According to Their Current Age, 2002–2004. Age 30 is 0.1% age 60 is 0.7% .
Jeffrey Dach MD
7450 Griffin Road
Davie, Fl 33314
954-792-4663
http://www.drdach.com
http://www.naturalmedicine101.com
http://www.truemedmd.com
Disclaimer click here: www.drdach.com/wst_page20.html
The reader is advised to discuss the comments on these pages with his/her personal physicians and to only act upon the advice of his/her personal physician. Also note that concerning an answer which appears as an electronically posted question, I am NOT creating a physician — patient relationship. Although identities will remain confidential as much as possible, as I can not control the media, I can not take responsibility for any breaches of confidentiality that may occur.
Link to this article:http://wp.me/P3gFbV-2x
Copyright (c) 2013 Jeffrey Dach MD All Rights Reserved. This article may be reproduced on the internet without permission, provided there is a link to this page and proper credit is given.
FAIR USE NOTICE: This site contains copyrighted material the use of which has not always been specifically authorized by the copyright owner. We are making such material available in our efforts to advance understanding of issues of significance. We believe this constitutes a ‘fair use’ of any such copyrighted material as provided for in section 107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section 107, the material on this site is distributed without profit to those who have expressed a prior interest in receiving the included information for research and educational purposes.
Pingback: google
Pingback: Russell Marker and the Origins of Bioidentical Hormones by Jeffrey Dach MD - Jeffrey Dach MD
Pingback: FDA Approval for Paxil for Hot Flashes A Cruel Joke ? - Jeffrey Dach MD
Pingback: The Safety of Bio-Identical Hormones by Jeffrey Dach MD - Jeffrey Dach MD
Pingback: Newsweek Attacks Oprah Winfrey and BioIdentical Hormones - Next Level Nutrition
Pingback: Synthetic Hormones Cause Breast Cancer - Jeffrey Dach MD
Pingback: Safety of Bioidentical Hormones - Jeffrey Dach MD
Pingback: New Attack on BioIdentical Hormones by Drug Industry - Jeffrey Dach MD
Pingback: Medical Conspiracies That Came True by Jeffrey Dach MD - Jeffrey Dach MD
Pingback: Hormone Replacement Therapy HRT Does NOT Cause Breast Cancer | Dr Colin Holloway
Pingback: More Lies about Bioidentical Hormones - Jeffrey Dach MD
Thank you Dr. Dach for all your work! and sharing of such important information. I’ve been taking bioidentical hormones since a total hysterectomy at age 37 in 1997. After a year of messing with synthetic hormones with no relief and terrible side effects, I persued finding a better option and did in compounded bioidentical hormones. Thank you for continuing to educate about the importance them.
Pingback: Why Bioidentical Hormones Are Safer Than Synthetic - Jeffrey Dach MD
Pingback: Jeffrey Dach MD New Attack on BioIdentical Hormones by Drug Industry - Jeffrey Dach MD